Part 2
‘Feline asthma’, sometimes referred to as ‘chronic bronchitis’ or ‘allergic airway disease’, is a term used to describe chronic lower airway disease affecting the small tubes (bronchioles) within the lungs of cats. In the first part in this article series, feline expert Elise Robertson explained what feline asthma is and how your vet will diagnose it.
Treatment Options
Anti-inflammatory Drugs
It is crucial to appreciate that widespread airway inflammation is responsible for the bronchoconstriction and mucous production in asthma cases. Therefore, anti-inflammatories, usually corticosteroids, have been the cornerstone treatment in attempts to reduce this inflammation. Corticosteroids can be given orally, by injection, or more recently via metered dose inhaler. Cats are more sensitive to potential side effects from injectable formulations as these are much more potent compared to tablet medications. This means that injections can only be given periodically, to reduce the risk of developing diabetes mellitus. Because long-term corticosteroid use has a potential risk of side effects (excessive urination, drinking more, diabetes, and more susceptible to infection), it is important that the dose is tapered over time in order to achieve the minimum dose to control the clinical signs and thus further reduce the chance of potential side effects. If higher doses are used indefinitely, the symptoms may become resistant to steroids. This phenomenon appears to be more common with injectable steroids with a shorter and shorter interval between injection times.
Inhaled steroids can be used in cats and are usually delivered using metered-dose inhalers (MDIs) with a spacing device. Many cats tolerate the facemask associated with spacing devices and some offer the advantage of including an indicator strip which ‘flutters’ when breaths are taken and medication is inhaled from the chamber. The major advantage to inhaled medications compared to oral and injectable treatments, is that the steroid is delivered directly to the lungs and systemic absorption is minimised thus reducing potential risks of side effects on other body systems.
Figure 1: Your veterinary surgeon will advise you on the best treatment option if your cat has asthma.
Bronchodilators
These drugs are used to relax the smooth muscles surrounding the bronchioles (small airway tubes) and help them dilate. These can be used during an acute crisis and also with corticosteroids. These are available in oral, injectable and inhaled formulations.
Terbutaline and theophylline are airway dilators commonly used in the management of asthma. Theophylline appears to be less effective in cats compared to dogs. A terbutaline injection, administered by your vet, can be extremely useful for an emergency situation when your cat is less likely to tolerate oral medications or masked medications.
Are there any other treatment options?
Other medications that might be helpful include:
Cyproheptadine
One of the chemicals involved in the inflammation cascade in feline asthma is called serotonin and appears to be directly involved in bronchoconstriction (airway narrowing) in cats. Cyproheptadine is an anti-serotonin medication with concurrent antihistamine properties. It can be used concurrently with steroids or in those where corticosteroid use is contraindicated; however their genuine value in these cases remains unclear.
Antihistamines
Histamine is an inflammatory mediator released during an allergic response. Histamine has been thought to have a contributory effect on airway constriction mechanisms. Despite being prescribed in these cases, recent research indicates that a certain receptor in the feline airway (called an H3 receptor) leads to a dilation when exposed to histamine rather than constriction. This may explain why antihistamines have not been found to be of dramatic use in managing feline asthma. Antihistamines have largely fallen out of favour compared to other more widely used medications.
Zamflurkast
This relatively new medication inhibits a chemical mediator called leukotrienes. It has received a lot of attention in the management of human asthma and its intended use is to complement other treatments with the aim of reducing the reliance on corticosteroids. It is still fairly experimental in cats and although many anecdotal reports appear favourable, more work is required to help clarify its potential value in feline asthma.
Inhalers for Cats…Are you Serious?
Human asthmatics have valued the benefits of having portable inhalers to manage their condition. These devices deliver medication locally to the airways and thus minimise potential side effects related to systemic medications.
Two main issues were discovered when using these devices in cats:
- Cats cannot be told when to breathe
- Cats tend to object to the spray of the medication actuation
Interestingly these same problems apply to human infants with asthma and a device called a paediatric spacer was therefore invented. The MDI fits to the end of the tubular ‘spacer’, and a face mask on the other. The inhaler is depressed, or ‘actuated’, into the spacer chamber and the infant, or in this case the cat, simply breathes in the aerosolised medication. One or two puffs, depending on what your vet has prescribed, are delivered into the chamber and then the face mask is gently held over your cat’s nose and mouth, allowing them to breathe the medication for approximately 10-15 seconds.
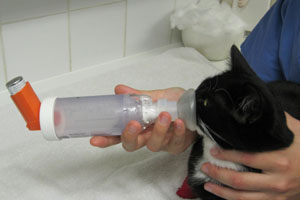
Figure 2: This patient was diagnosed with feline asthma. He is receiving inhaled medications using a spacing chamber. This allows a cat to inhale much needed medications for 20-30 seconds.
Corticosteroid inhalers are typically used twice daily long term while airway dilator inhalers such as albuterol-containing inhalers (bronchodilators) are used to manage acute flare-ups.
Cats are generally started on a combination of oral corticosteroids and inhaled steroids. The oral medications are gradually weaned down and then maintained on only the metered dose inhaler. A device created specifically for feline use can be ordered from your veterinary surgeon. It comes with the spacer and different sized face masks.

Figure 3: It is important that cats with asthma are not exposed to cigarette smoke
My cat has been diagnosed with feline asthma/bronchitis. What is the prognosis?
The prognosis depends mainly on the severity of disease and overall response to treatment(s). In many cases, appropriately prescribed medications/treatment will dramatically improve clinical signs and quality of life for your cat. This is considered a life-time condition and will need to be monitored and managed promptly during acute attacks as this can be life-threatening. Some severe cases may have very little functional lung tissue remaining due to scar tissue formation in the lungs – a condition called pulmonary fibrosis. Unfortunately, very little can be done for pulmonary fibrosis as these changes are considered to be irreversible.
In Summary…
Minimising airborne irritant exposure is essential.
- Do not allow cigarette smoke in the cat’s environment
- Use dustless cat litter
- Refrain from using aerosol sprays and powders in the cat’s environment
- Do not use scented candles/incense sticks
It is vital to understand that asthma can culminate in a life-threatening respiratory crisis. Do not ignore signs of fast laboured breathing/open-mouth breathing! Contact your local veterinary surgery immediately.
 The Veterinary Expert| Pet Health
The veterinary expert provides information about important conditions of dogs and cats such as arthrits, hip dysplasia, cruciate disease, diabetes, epilepsy and fits.
The Veterinary Expert| Pet Health
The veterinary expert provides information about important conditions of dogs and cats such as arthrits, hip dysplasia, cruciate disease, diabetes, epilepsy and fits.
 The Veterinary Expert| Pet Health
The veterinary expert provides information about important conditions of dogs and cats such as arthrits, hip dysplasia, cruciate disease, diabetes, epilepsy and fits.
The Veterinary Expert| Pet Health
The veterinary expert provides information about important conditions of dogs and cats such as arthrits, hip dysplasia, cruciate disease, diabetes, epilepsy and fits.